When actor Bruce Willis’s family publicly shared his diagnosis of frontotemporal dementia (FTD) in 2023, it brought global attention to a condition that millions of people had never heard of. While Alzheimer’s disease dominates public conversations about dementia, frontotemporal dementia is actually the most common form of early-onset dementia for individuals under 65. Despite its prevalence in younger populations, FTD remains widely misunderstood by the general public, medical professionals outside of neurology, and even some caregivers.
This guide provides a thorough overview of what frontotemporal dementia is, the symptoms and stages families should watch for, the underlying causes and risk factors, how the condition is diagnosed, and what treatment and management options are available. Whether you are a caregiver, a family member, or a medical professional seeking deeper knowledge, the information below will help you better understand and support those living with this challenging condition.
What Is Frontotemporal Dementia?
Frontotemporal dementia is a group of progressive brain disorders caused by the degeneration of nerve cells in the frontal and temporal lobes of the brain. These regions are responsible for personality, behavior, language, decision-making, and emotional regulation. As these lobes of the brain deteriorate, individuals experience profound changes that can affect virtually every aspect of daily life.
FTD is sometimes referred to by the broader medical term frontotemporal lobar degeneration (FTLD), which describes the underlying pathological process of nerve cell loss. Unlike Alzheimer’s disease, which is characterized by the accumulation of beta-amyloid plaques and tau tangles primarily affecting memory centers, frontotemporal degeneration targets the frontal lobe and temporal lobes specifically, leading to a distinct clinical presentation.
Frontotemporal disorders encompass several clinical subtypes, each with its own pattern of symptoms. The three main variants are behavioral variant frontotemporal dementia (bvFTD), semantic dementia (also called semantic variant primary progressive aphasia), and progressive nonfluent aphasia (also called nonfluent/agrammatic variant primary progressive aphasia). Additionally, some individuals develop movement-related disorders such as progressive supranuclear palsy, corticobasal syndrome, or FTD combined with amyotrophic lateral sclerosis (FTD-ALS, sometimes referred to as FTD-MND).
FTD is most commonly diagnosed in people between the ages of 45 and 65, making it a form of young-onset or early-onset dementia. However, it can occur in individuals as young as their 20s or as old as their 80s. Estimates suggest that FTD affects approximately 50,000 to 60,000 people in the United States, though the true number may be higher due to frequent misdiagnosis.
Frontotemporal Dementia Symptoms and Stages
The first symptoms of frontotemporal dementia depend largely on which parts of the brain are affected earliest. Unlike Alzheimer’s, where memory loss is typically the hallmark early symptom, FTD often begins with changes in behavior, personality, or language ability. Recognizing these first signs of frontotemporal dementia is critical for early intervention and family planning.
Behavioral Variant Frontotemporal Dementia (bvFTD)
Behavioral variant frontotemporal dementia is the most common subtype, accounting for roughly half of all FTD cases. People with bvFTD often display dramatic behavioral symptoms that are noticeable to family members and coworkers long before a formal dementia diagnosis is made.
Common behavioral symptoms include a loss of empathy or concern for others, socially inappropriate or impulsive behavior, apathy and withdrawal from activities once enjoyed, obsessive-compulsive behaviors or rigid routines, changes in eating habits such as overeating or craving sweets, and poor decision-making or judgment. Individuals may also display a lack of awareness of their own behavioral changes, which can be particularly distressing for family members who witness the transformation.
Primary Progressive Aphasia (PPA)
Primary progressive aphasia is a language-dominant form of FTD that progressively impairs a person’s ability to speak, read, write, or understand language. There are three recognized subtypes: semantic variant (semantic dementia), nonfluent or non-fluent/agrammatic variant, and logopenic variant. Each presents with distinct language problems.
In semantic dementia, individuals gradually lose the meaning of words and concepts. They may speak fluently but use vague or incorrect words. In the nonfluent variant, speech becomes halting and effortful, with grammatical errors and difficulty forming sentences. The logopenic variant is characterized by word-finding difficulties and slow speech, though grammar and comprehension may remain relatively intact in the early stages.
Speech-language pathologists play an important role in evaluating and supporting individuals with progressive aphasia, helping to develop strategies that maintain communication for as long as possible.
Movement-Related Symptoms
Some forms of frontotemporal dementia also produce movement-related symptoms similar to those seen in Parkinson’s disease or motor neuron disease. Progressive supranuclear palsy causes problems with balance, eye movement, and swallowing. Corticobasal syndrome leads to stiffness, difficulty with coordinated movements, and sometimes an inability to control a limb. FTD-ALS (also called FTD-MND) combines cognitive and behavioral symptoms with the muscle weakness and wasting characteristic of amyotrophic lateral sclerosis. Some individuals with FTD may also lean forward or develop postural instability as the disease progresses.
The 7 Stages of Frontotemporal Dementia
While the progression of FTD varies significantly from person to person, clinicians and caregivers often describe it in seven general stages. In the early stages, individuals may show subtle personality changes or mild language problems that are easily overlooked. As the disorder progresses through moderate stages, behavioral symptoms and communication difficulties become more pronounced, and the person may need increasing assistance with daily tasks. In the advanced stages, individuals typically require full-time care, experience significant physical decline, and may lose the ability to speak, walk, or swallow independently.
It is important to note that FTD does not follow a rigid progression. Some people may remain relatively stable for years, while others decline more rapidly. The specific subtype, the individual’s overall health, and the presence of other conditions such as ALS all influence the pace of decline.
How Does Someone with Frontotemporal Dementia Act?
One of the most challenging aspects of frontotemporal dementia for family members is the dramatic change in how a person acts. Because the frontal lobe governs social behavior, impulse control, and emotional regulation, individuals with FTD may behave in ways that seem entirely out of character.
A person who was once empathetic and socially aware may become rude, disinhibited, or indifferent to the feelings of others. They may make inappropriate comments in public, engage in compulsive behaviors like hoarding or repetitive movements, or lose interest in personal hygiene. Some individuals develop obsessive-compulsive tendencies, while others become passive and apathetic, showing little motivation or initiative. These changes are not voluntary—they are the direct result of neurological damage to parts of the brain that regulate behavior and personality.
Frontotemporal Dementia Causes and Risk Factors
The causes of frontotemporal dementia are rooted in the abnormal accumulation of certain proteins in the brain’s nerve cells. The two most commonly implicated proteins are tau and TDP-43. When these proteins misfold and aggregate, they disrupt normal cell function and eventually cause nerve cell death in the frontal and temporal lobes. Less commonly, FTD can be associated with proteins related to FUS (fused in sarcoma).
Unlike Alzheimer’s disease, which is strongly associated with beta-amyloid plaques, frontotemporal dementia does not typically involve amyloid pathology. This distinction is important because it means that diagnostic tests and treatments designed for Alzheimer’s are generally not applicable to FTD.
Genetic Factors and Family History
Genetics play a more prominent role in FTD than in many other forms of dementia. Approximately 30 to 50 percent of individuals with FTD have a significant family history of the disease or related neurological conditions. Mutations in several genes have been identified, including the MAPT gene (which encodes the tau protein), the GRN gene (which produces progranulin), and the C9orf72 gene (associated with both FTD and ALS).
For families with a known history of frontotemporal dementia, genetic testing and genetic counseling can provide valuable information about the likelihood of developing the disease. However, it is important to understand that a genetic mutation does not guarantee disease onset, and the decision to pursue genetic testing is deeply personal. Consulting with a genetic counselor can help individuals and family members weigh the potential benefits and emotional impact of testing.
Who Is Most Likely to Get Frontotemporal Dementia?
FTD does not discriminate by gender or ethnicity, though some studies suggest slight variations in subtype prevalence. The strongest known risk factor is a family history of FTD or related disorders. People who usually get frontotemporal dementia are between 45 and 65, though the condition can appear at any age. Unlike Alzheimer’s, advanced age is not a primary risk factor for FTD, which is why it is classified as an early-onset or young-onset dementia.
How Is Frontotemporal Dementia Diagnosed?
Diagnosing frontotemporal dementia is often a complex and lengthy process. Because the early symptoms of FTD can mimic psychiatric conditions such as depression, bipolar disorder, or obsessive-compulsive disorder, many individuals receive an incorrect initial diagnosis. On average, it takes roughly three to four years from the onset of symptoms to receive an accurate FTD dementia diagnosis.
Clinical Evaluation and Neuropsychological Testing
The diagnostic process typically begins with a thorough clinical evaluation by a neurologist or behavioral neurologist. This includes a detailed medical and family history, interviews with the patient and family members, and standardized neuropsychological assessments. Neuropsychological testing evaluates cognitive functions such as memory, language, attention, problem-solving, and social cognition, helping to identify patterns that distinguish FTD from Alzheimer’s or other conditions.
Brain Imaging: Does Frontotemporal Dementia Show on MRI?
Brain imaging plays a vital role in the diagnosis of FTD. Magnetic resonance imaging (MRI) can reveal characteristic patterns of atrophy (shrinkage) in the frontal and temporal lobes. In behavioral variant FTD, the frontal lobe is typically more affected, while language variants may show more prominent temporal lobe atrophy. However, in the early stages of FTD, the MRI may appear normal or show only subtle changes, which is one reason why misdiagnosis is common.
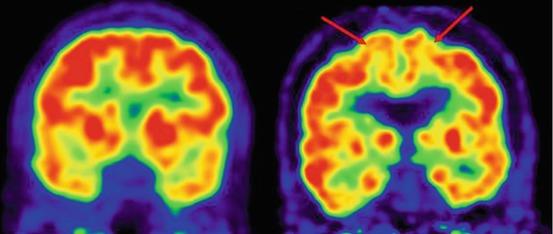
Positron emission tomography (PET) scans can also be helpful, as they detect reduced metabolic activity or blood flow in affected brain regions. In some cases, amyloid PET scans are used to rule out Alzheimer’s disease by confirming the absence of beta-amyloid deposits. Additionally, research efforts supported by the National Institute of Neurological Disorders and Stroke and other National Institute agencies are working to develop more sensitive biomarkers for earlier detection.
Genetic Testing
For individuals with a family history of FTD, genetic testing can identify known mutations associated with the disease. While genetic testing cannot confirm a clinical diagnosis of FTD on its own, it can be a powerful tool when combined with other diagnostic data. It also has implications for other family members who may want to understand their own risk.
What Is the Life Expectancy of Someone with Frontotemporal Dementia?
The life expectancy of someone with frontotemporal dementia varies widely depending on the subtype, the rate of progression, and the presence of co-occurring conditions. On average, people live six to eight years after the onset of symptoms, though some may live longer than a decade and others, particularly those with FTD-ALS, may have a more rapid decline.
The life expectancy of someone with frontal lobe dementia is similarly variable. Because the disease affects relatively younger individuals, comprehensive support, good nutrition, physical activity, and attentive medical care can help maintain quality of life and may influence overall survival.
Treatment and Management of Frontotemporal Dementia
There is currently no cure for frontotemporal dementia, and no medications have been specifically approved to treat it. However, a multidisciplinary approach to care can help manage symptoms and improve quality of life.
Medications originally developed for other conditions are sometimes used off-label to address specific symptoms. Selective serotonin reuptake inhibitors (SSRIs) may help reduce compulsive behaviors and improve mood. Antipsychotic medications are occasionally used with caution for severe agitation or psychosis, though they carry significant risks in dementia patients.
Non-pharmacological approaches are equally important. Speech-language therapy can help individuals with primary progressive aphasia maintain communication skills. Occupational therapy supports daily functioning, and physical therapy addresses balance and mobility challenges. Behavioral interventions, including environmental modifications and structured routines, are often the most effective strategies for managing the behavioral symptoms of FTD.
Bruce Willis’s Diagnosis and Its Impact on Awareness
In March 2022, Bruce Willis’s family announced that the beloved actor was stepping away from his career after being diagnosed with aphasia, a language disorder that impacts communication. By February 2023, the family shared that his condition had progressed to frontotemporal dementia, putting a public face on a condition that had previously received limited media attention.
Since then, his wife Emma Heming Willis and his daughters have used their platform to raise awareness about FTD, sharing updates with compassion and honesty. Their advocacy has highlighted that dementia does not only affect memory—it can profoundly alter communication, personality, relationships, and daily life. Willis’s story has also underscored the importance of early detection, proper diagnosis, and support for both patients and their families.
The visibility brought by Willis’s diagnosis has contributed to increased funding for FTD research and greater public engagement with organizations like the Association for Frontotemporal Degeneration (AFTD), which provides education, support groups, and advocacy for families affected by the disease.
Supporting a Loved One with FTD
For families, an FTD diagnosis can feel overwhelming. The progressive nature of the disease, combined with the often-young age of those affected, creates unique emotional, financial, and logistical challenges. However, there are meaningful ways to support a loved one and maintain the highest possible quality of life.
Creating structure and routine helps reduce anxiety and confusion. Using clear, simple communication—short sentences, visual cues, and a calm tone—supports ongoing connection. Focusing on emotional presence rather than correcting errors in speech or behavior preserves the bond between caregiver and loved one.
Connecting with support groups through organizations like the AFTD, the Alzheimer’s Association, and local caregiver networks provides invaluable emotional support and practical guidance. Many families also benefit from respite care, which gives caregivers time to recharge while ensuring their loved one receives attentive, professional support.
Specialized memory care communities offer environments tailored to the unique needs of individuals with FTD. These communities provide structured programming, compassionate staff trained in dementia care, and a safe setting that promotes independence and dignity at every stage of the journey.
A Message of Compassion and Hope
Bruce Willis’s journey reminds us that a dementia diagnosis does not define a person. Behind every diagnosis is a lifetime of love, laughter, and meaningful connections. By sharing his story, his family has not only illuminated a lesser-known form of dementia but also inspired millions to show more compassion and support for those living with cognitive changes.
Ongoing research continues to deepen our understanding of frontotemporal degeneration, and clinical trials are exploring new therapeutic approaches. While a cure remains on the horizon, advances in early detection, genetic testing, and symptom management offer genuine reasons for hope.
At Azura Memory Care, we are honored to walk alongside families on this journey, providing personalized care rooted in empathy, respect, and purposeful living. Whether you are seeking information, support, or a caring community for a loved one, we are here to help.

